All HCCI Reports
HCCI’s original reports powered by #HCCIdata
-
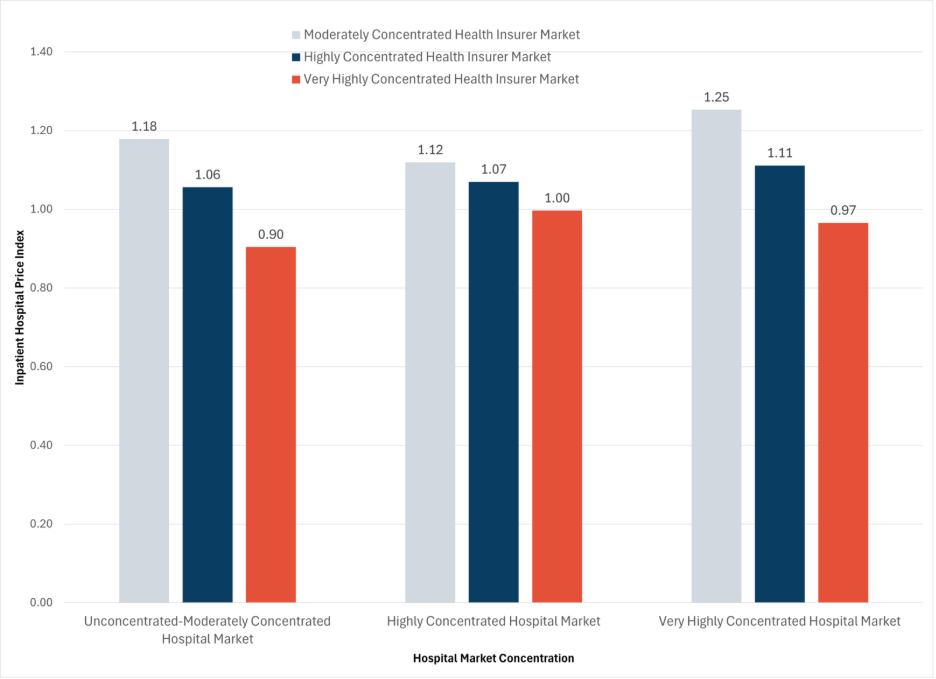
Inpatient Hospital Prices are Highest Where Hospital Competition is Lowest
 Read more: Inpatient Hospital Prices are Highest Where Hospital Competition is Lowest
Read more: Inpatient Hospital Prices are Highest Where Hospital Competition is LowestConventional wisdom and economic theory suggest that more competition means lower prices. In health care, there is longstanding evidence that geographic areas with less competition among hospitals are associated with higher negotiated commercial prices. Regulators and researchers use the Herfindahl-Hirschman Index (HHI) to measure market concentration at a geographic area. HHI can range from 0 (competitive market) to 10,000 (monopoly market). Hospital markets that are considered “highly concentrated,” (HHI greater than…
-
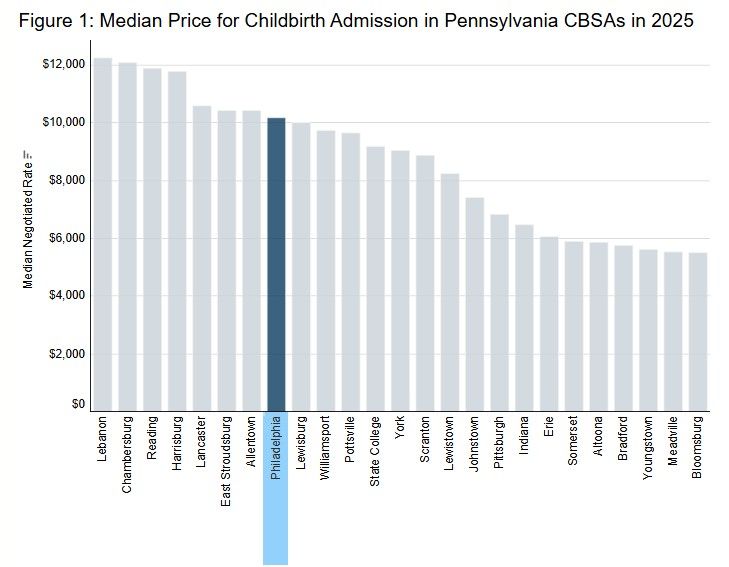
Transparency Data Highlight Wide Variation in the Price of Childbirth
 Read more: Transparency Data Highlight Wide Variation in the Price of Childbirth
Read more: Transparency Data Highlight Wide Variation in the Price of ChildbirthChildbirth is the most common reason for an inpatient hospital admission among people with employer-sponsored insurance. Despite how routine it is, the price of giving birth can vary widely depending on where you live, which hospital you use, and which insurer you have. Using Transparency in Coverage (TiC) data, we set out to better understand…
-
Leveraging Transparency in Coverage (TiC) Data for Health Care Price Analysis
 Read more: Leveraging Transparency in Coverage (TiC) Data for Health Care Price Analysis
Read more: Leveraging Transparency in Coverage (TiC) Data for Health Care Price AnalysisThe Transparency in Coverage (TiC) regulations have introduced unprecedented visibility into negotiated health care prices in the United States. By requiring insurers to publish machine-readable files containing payer–provider contracted rates starting in 2022, the policy has created a new data source for studying price variation. However, the scale, inconsistency, and missing information within the TiC…
-
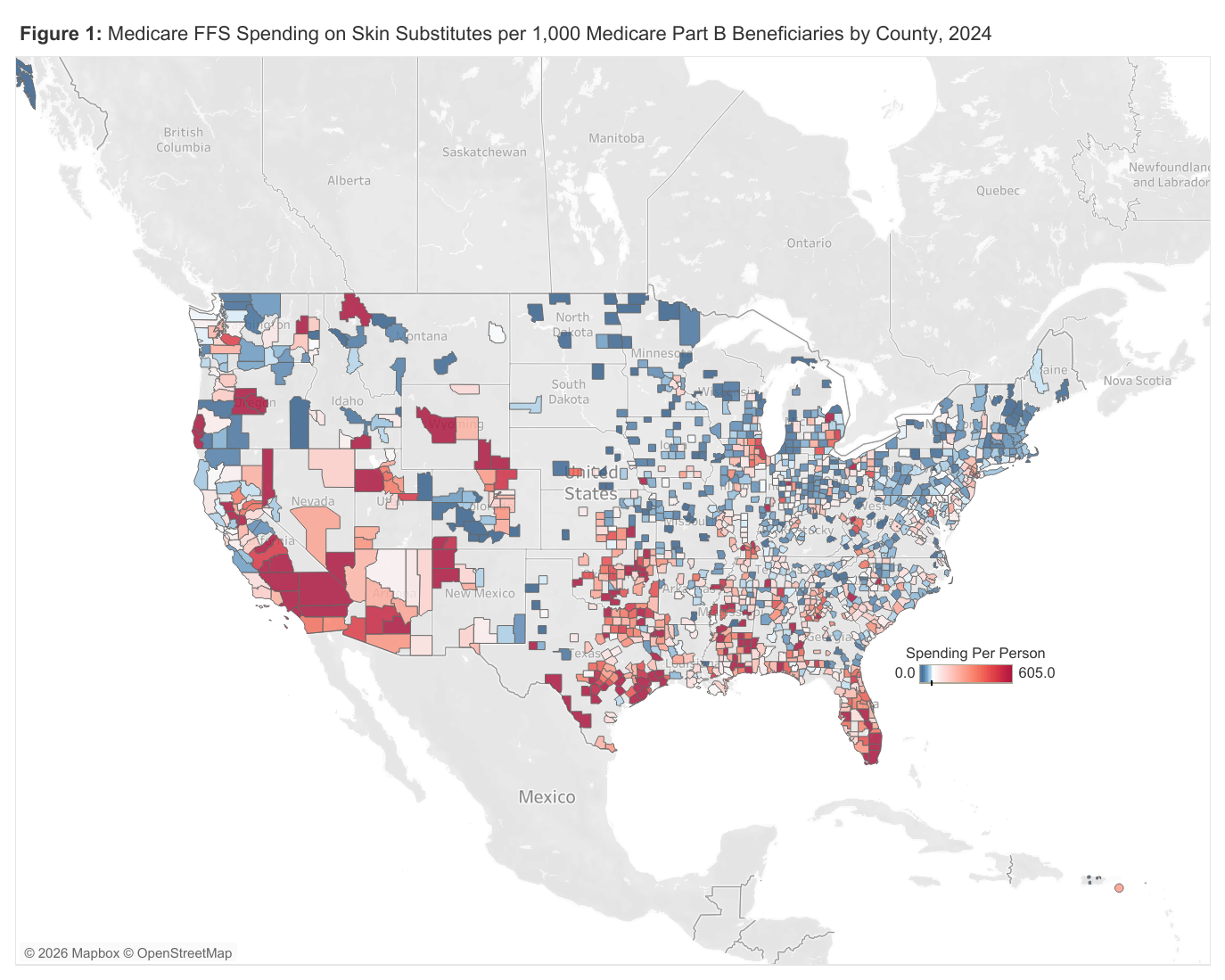
High Medicare Spending on Skin Substitutes Is the Result of Higher Prices, More Patients, and More Products
 Read more: High Medicare Spending on Skin Substitutes Is the Result of Higher Prices, More Patients, and More Products
Read more: High Medicare Spending on Skin Substitutes Is the Result of Higher Prices, More Patients, and More ProductsSkin substitutes have gained attention recently for the rapid growth in Medicare Part B spending. Used to replace or regenerate damaged skin, skin substitutes are bioengineered materials or tissue products that mimic the structure and function of healthy skin and can serve as a permanent or temporary solution to conditions like diabetic foot ulcers or burns. …
-
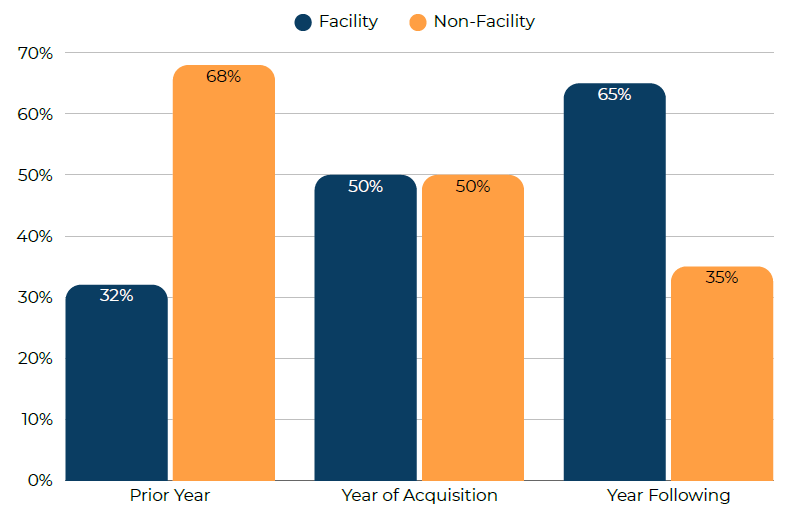
Effects of Vertical Integration on Providers’ Billing and Practice Patterns in ESI (2018-2022)
 Read more: Effects of Vertical Integration on Providers’ Billing and Practice Patterns in ESI (2018-2022)
Read more: Effects of Vertical Integration on Providers’ Billing and Practice Patterns in ESI (2018-2022)In this report, we study changes in billing and practice patterns following providers’ acquisition by health systems, from 2018 to 2022, using HCCI’s unique dataset of people with employer-sponsored insurance. First, we looked at Evaluation and Management (E&M) visits to see if providers that had been acquired billed higher intensity visits following acquisition, which could…
-
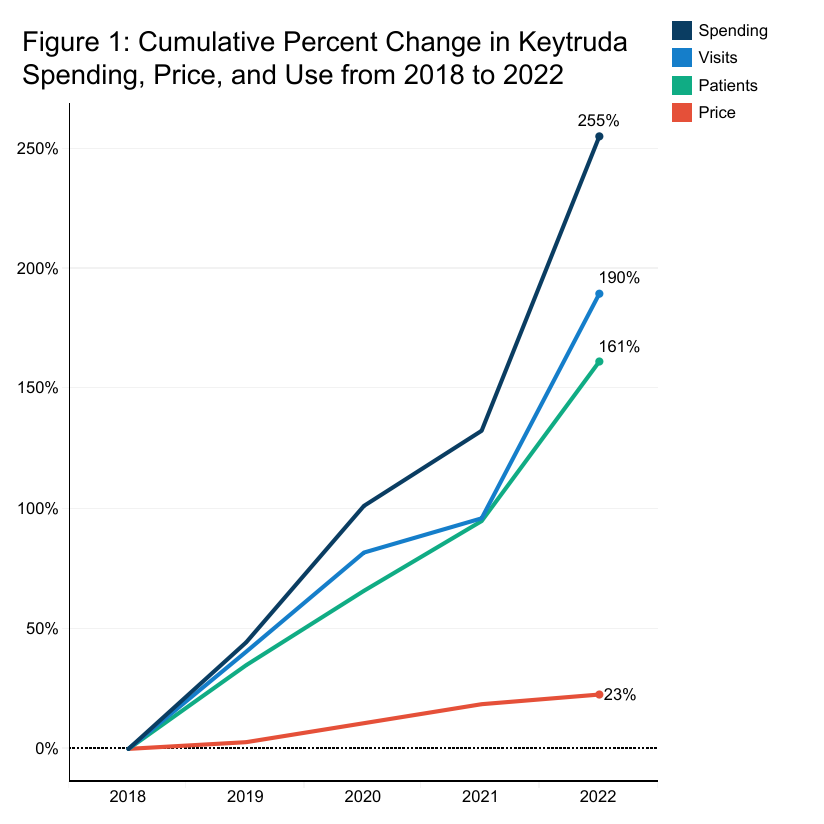
Keytruda: How Expanding Use and Site-of-Service Prices Made Keytruda the Top Spending Administered Drug
 Read more: Keytruda: How Expanding Use and Site-of-Service Prices Made Keytruda the Top Spending Administered Drug
Read more: Keytruda: How Expanding Use and Site-of-Service Prices Made Keytruda the Top Spending Administered DrugIn 2021, Keytruda (pembrolizumab) became the highest-spending clinician-administered drug among the commercially insured population (people under age 65 covered through employer-sponsored insurance). Keytruda is an immune checkpoint inhibitor (anti–PD-1 monoclonal antibody) administered by infusion and used across a growing number of cancers, often in combination with chemotherapy or other agents and in both metastatic and…
-
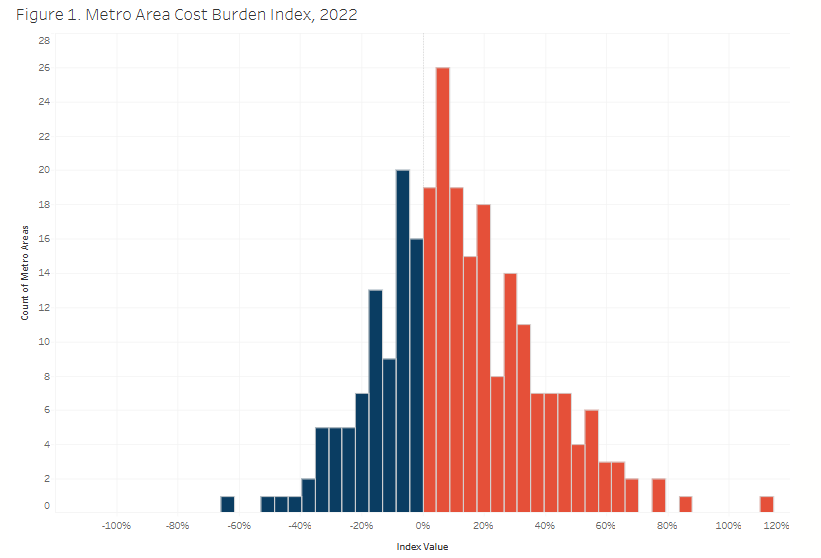
Health Cost Landscape Highlights How Health Care Spending and Income Shape Cost Burden and Affordability
 Read more: Health Cost Landscape Highlights How Health Care Spending and Income Shape Cost Burden and Affordability
Read more: Health Cost Landscape Highlights How Health Care Spending and Income Shape Cost Burden and AffordabilityThe Health Cost Landscape is an interactive tool created by the Health Care Cost Institute that uses data from employer-sponsored insurance plans to compare health care spending, prices, use, and service mix across 269 metro areas and 45 states. The Landscape tool shows that health care spending varies widely across the United States, ranging from…
-
The Health Cost Landscape: Different Costs, Different Drivers Across U.S. Markets
 Read more: The Health Cost Landscape: Different Costs, Different Drivers Across U.S. Markets
Read more: The Health Cost Landscape: Different Costs, Different Drivers Across U.S. MarketsThe Health Cost Landscape is an interactive tool created by the Health Care Cost Institute that provides data on health care spending, including the use, price, and mix of services for 269 individual metro areas across 45 states. This brief highlights key findings from the Health Cost Landscape’s analysis of local areas across the country.
-
What is the Health Cost Landscape?
 Read more: What is the Health Cost Landscape?
Read more: What is the Health Cost Landscape?The Health Cost Landscape is an interactive tool created by the Health Care Cost Institute (HCCI) that provides metro area and state-level data on health care spending. It breaks down the factors that contribute to spending, including the use, prices, and mix of services that people in an area receive. The Health Cost Landscape website…
-
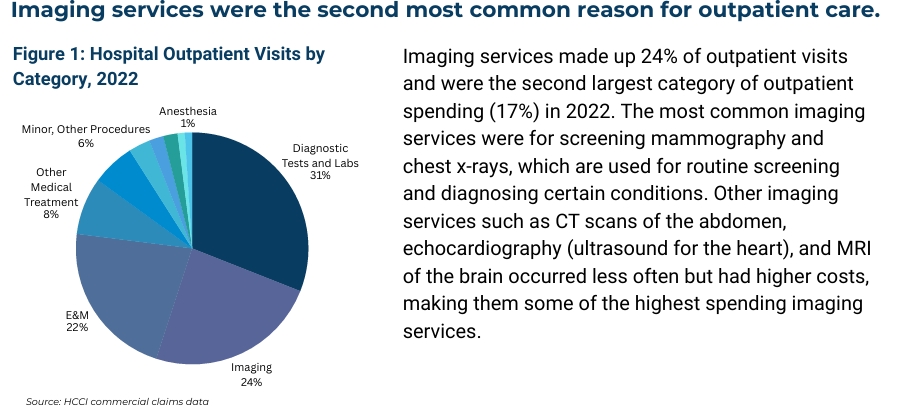
Issue Brief: Imaging Services are the Second Most Common Outpatient Service
 Read more: Issue Brief: Imaging Services are the Second Most Common Outpatient Service
Read more: Issue Brief: Imaging Services are the Second Most Common Outpatient ServiceAcross several HCCI analyses, imaging services have emerged as commonly used services that account for a significant amount of spending, specifically in hospital outpatient department settings. This brief highlights the use and price of imaging services in hospital outpatient settings among people with employer-sponsored insurance (ESI).

